It’s become common knowledge that the elderly and people who are immunocompromised are at increased risk of severe illness from coronavirus.
But there’s another underlying condition that millions of Americans have that helps place the country at first place in coronavirus cases compared to the rest of the world and that medical professionals say may be leading to increased risk of severe illness — obesity.
The obesity rate in the U.S. is roughly 38%, a number that makes Americans the heaviest in the world. According to the Centers for Disease Control and Prevention, people of any age that are obese are at increased risk of severe illness from COVID-19.
The comparison between the U.S.’s obesity rate and the rest of the world’s is striking. In Europe, Hungary was among the only countries to come close to the U.S.’s rate, at 30%. Mexico was the second heaviest, at 32.4%, according to Market Watch.
Medical professionals like Dr. Stephen J. Carter have questioned the links between obesity and coronavirus complications. While experts continue to learn more about the links between the two, there has been evidence indicating that one of America’s epidemics — obesity — is worsening the effects of the pandemic for Americans who are obese.

DES PLAINES, IL – JUNE 13: A heavyset man passes cartons of Coca-Cola displayed in a grocery June 13, 2006 in Des Plaines, Illinois. Doctors at the annual American Medical Association meeting in Chicago this week have called for a “fat tax” on sugary soft drinks to help fight obesity in the U.S. (Photo by Tim Boyle/Getty Images)
“We have long-recognized that obesity is associated with greater vulnerability and attendant consequences from viral infection. Thus, amid the COVID-19 pandemic, what we are witnessing is unsurprising as compelling evidence indicates people living with obesity are at greater risk for health complications from SARS-CoV-2,” Carter told the Daily Caller.
“Symptom-severity appears to be more virulent among those with obesity, but the mechanisms accounting for this link are incompletely understood. Chronic low-grade inflammation coupled with reduced regulatory T cell frequency and poorer vascular health have been implicated.”
Dr. William Dietz, the director of the Sumner M. Redstone Global Center for Prevention and Wellness at George Washington University and the director of the STOP Obesity Alliance, says that these mechanisms remain uncertain, but that the increase of respiratory effort required by people with obesity is one factor that may contribute to the severity of coronavirus for people with obesity infected with it.
The physical properties of obesity, especially if a patient is placed in a supine position, meaning lying horizontally with the face and torso facing up, may also make it harder for people with obesity to breathe if they have been hospitalized with COVID-19 because the fat pushed the diaphragm up even further.
“The increase of respiratory effort required by people with obesity, one is the intra-abdominal fat means that when you breathe your diaphragm has to push against that fat to get an adequate volume of air.”
Conditions associated with obesity, like diabetes, are also listed as medical conditions that increase the risk of severe illness.
“If you look at the data of other disease exposures people with more severe course of COVID 19 have hypertension, diabetes, things like that, which are associated with obesity,” Dietz tells the Caller.
Carter adds that while causation can not yet be determined, obesity paired with an existing condition like hypertension or diabetes may be compound COVID-19 severity.
“Symptom severity and management appear to be exacerbated in the setting of hypertension and diabetes – both of which are typically connected to obesity. Though we cannot determine causation, it is reasonable that in the setting of obesity, having an existing comorbidity like hypertension and/or diabetes may contribute to a protracted burden from SARS-CoV-2.”
More than 100 million U.S. adults had diabetes or prediabetes, according to a CDC report in 2017. 30.3 million Americans, or 9.4% of the population, had diabetes in 2017 with a steady rate of diagnoses. A 2020 report showed that the number increased to 34.2 million people with diabetes, which is 10.5% of the population, and 7.3 million people are undiagnosed.
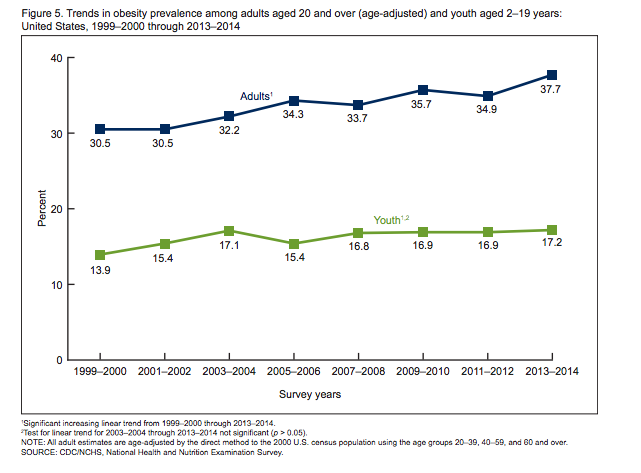
Obesity rates in U.S. adults and children from 1999-2014 (Image: Centers for Disease Control and Prevention)
The COVID-NET report, published by the Centers for Disease Control and Prevention in April, also found that of the patients who’d contracted coronavirus, 9 out of 10 of them had an underlying health condition. Of those patients, 48.3% were obese. (RELATED: Hospital Analysis Reports Show Nearly Half Of Coronavirus Patients Are Obese)
“We recognize that prognosis tends to be worse when an individual is presenting an exaggerated pro-inflammatory immune response. This, in turn, confounds proper cardiac and pulmonary function,” Carter adds.
Dietz says that some studies in Europe have shown an association with obesity and COVID-19, but he hasn’t seen data aside from the mortality data showing the differences in obesity accounting for differences in mortality across countries, and believes that the response to the pandemic is responsible for some disparity.
Furthermore, he says COVID-19 mortality data doesn’t currently show the breakdown accounting for the different diseases associated with obesity.
“The ideal study would show mortality associated with obesity, with or without diabetes, with or without hypertension. I’m not sure it tells us any more about the role of obesity in COVID-19 mortality.”
Carter adds that while researchers try to develop a vaccine for COVID-19, Americans should be reminded that a healthy lifestyle can help promote “systemic health benefits.”
“While researchers move toward an efficacious vaccine for SARS-CoV-2, we should be reminded that embracing healthy behaviors like consuming a well-rounded diet and exercising promote systemic health benefits. Such behaviors may preemptively support immune homeostasis and attenuate symptom severity.”
A question that remains unanswered, he says, relates to how people with obesity could respond to a vaccine when it’s available.
“What remains unclear is how people with obesity may respond differently to novel therapeutics seeking to treat/prevent symptom complications from SARS-CoV-2.”


