A new mass study of VA patients found that individuals who survive COVID-19 are more likely to experience a variety of cardiovascular issues down the line.
In the study, published Feb. 7 in Nature Medicine, researchers examined health outcomes for patients who contracted COVID-19 between March 2020 and January 2021 in the Veterans Affairs healthcare database and compared them to cohorts from the same time period who did not catch COVID-19, as well as a cohort from prior to the pandemic. They found that COVID-19 patients faced higher risk of conditions including heart failure, stroke, dysrhythmia, pericarditis, myocarditis, cardiac arrest and more one year after infection.
On the whole, veterans who had COVID-19 had a 72% higher risk of heart failure and 63% higher risk of any negative cardiovascular outcome than those who didn’t have the virus. However, there are some caveats within the data.
The population studied consists of only veterans, and thus skews heavily male, white and older. The average age of the patients studied was early 60s, 90% were men and about three-quarters were white.
There were some risk factors that produced worse outcomes. Patients over age 65 faced more significant risk increases for most conditions, including major adverse cardiac events (MACE) like strokes and mortality-inducing conditions. Men faced a higher risk increase for all types of conditions studied, as did smokers. Patients with pre-existing comorbidities like diabetes, obesity or already-present heart disease faced lower increases of risk, presumably because their risk of heart issues was higher to begin with.
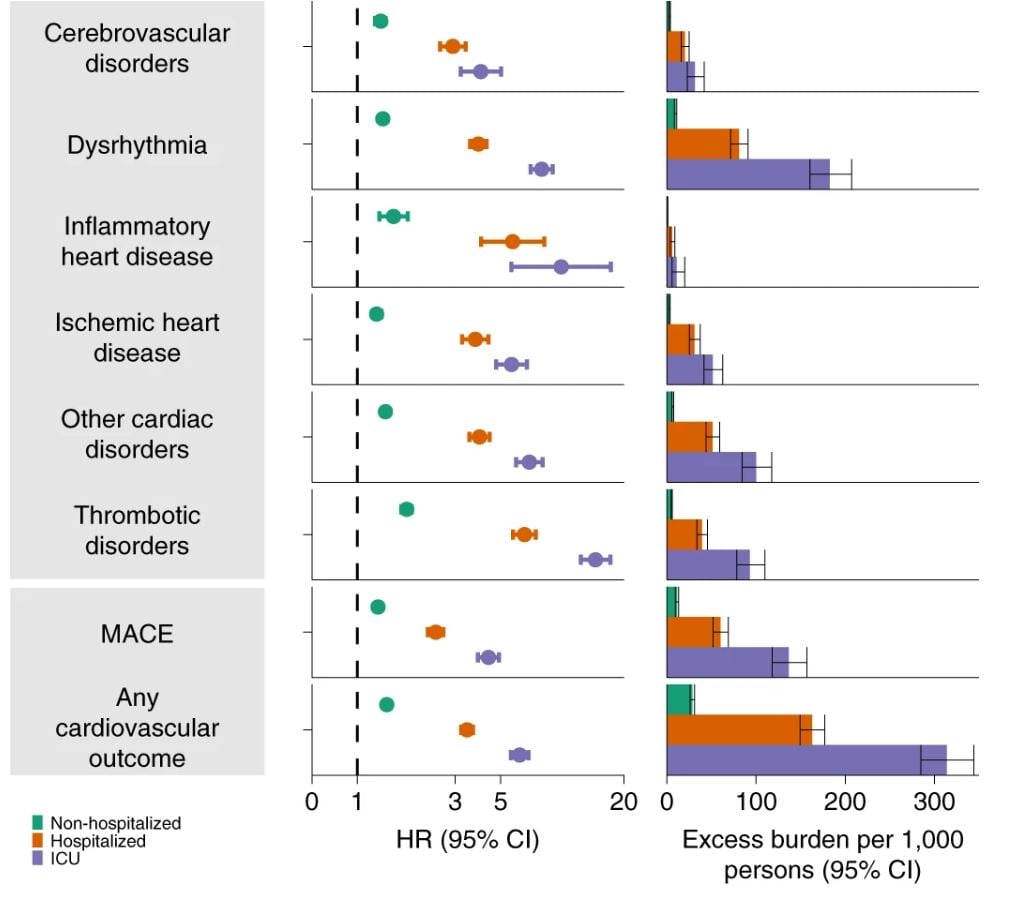
A figure shows the increased risk of heart conditions from catching COVID-19 depending on severity of case. (Screenshot/Nature Medicine)
Risk increases also correlated significantly with the severity of COVID-19 infection. For patients who were not hospitalized, there was still a higher risk of developing heart problems, but it ranged from one-half to less than one-tenth the risk increase for patients who were in the ICU.
The only conditions for which non-hospitalized patients faced a doubling of risk or worse were pulmonary embolism and myocarditis, the latter of which saw the highest increase of risk for all groups. (RELATED: CNN Medical Analyst Says Mask Mandate Should End Because ‘Science Has Changed.’ But Has It?)
For some conditions, like cardiac arrest, cardiogenic shock and myocardial infarction, risk for non-hospitalized patients was indistinguishable from risk for individuals who didn’t get COVID-19 at all. Overall, the excess burden for every condition except myocarditis was drastically higher for patients who were hospitalized and put in ICUs than non-hospitalized patients.
Additionally, given the timing of the study, virtually all infections occurred before COVID-19 vaccines were available in the United States.
The sample of COVID-19-infected patients totaled 153,760. The contemporary cohort of uninfected patients totaled 5,637,647, and the historical cohort of patients from 2017 totaled 5,859,411.