Despite several reporting protocols designed to prevent fraud, Medicaid has doled out $161 billion in improper payments since 2008.
Individuals falsifying information to meet qualification requirements, filing false claims and visiting multiple providers for the same condition in addition to fraud committed by providers is creating a huge financial strain on the country, a study given to The Daily Caller News Foundation conducted by American Action Forum (AAF) – a Washington, D.C.-based, center-right think tank — found.
According to AAF’s calculations using the Congressional Budget Office’s most recent budget projections, eliminating all waste, fraud and abuse in the entitlement program, which has seen a 25 percent increase in enrollment since 2013 and a 16 percent rise in federal expenditures in 2015 – would bring down the deficit by around 11.4 percent.
“In 2014, 6.7 percent of all Medicaid payments were improper, causing Medicaid to be responsible for 14 percent ($17.5 billion) of all federal improper payments, second only to Medicare, which was responsible for 49 percent of federal improper payments,” the study reads. “In 2015, Medicaid’s improper payment rate (IPR) increased by nearly half to 9.78 percent or $29 billion.”
The payments – which account for 17 percent of all the federal government’s improper payments – were more often provided to those treated through fee-for-service, which was expanded under the Affordable Care Act, with 10.6 percent receiving payments versus the .14 percent of those enrolled in the entitlement program’s managed care programs.
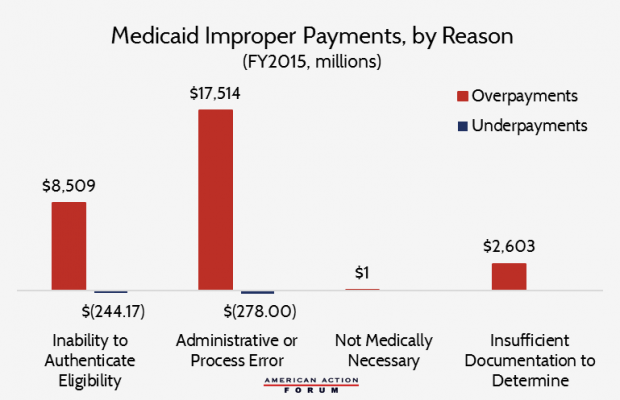
AAF
The group said the issue is partially due to many of the tools aimed at preventing fraud being optional for states.
“Because reporting information consumes already-limited resources, and states have historically had little incentive to recover improper payments—due to the fact that for each dollar recovered, states may only keep their share of the funding (which is always less than half)—many states choose to not report,” the study says.
AAF said a “complete and accurate national Medicaid database” would help eliminate the problem.
The group also highlighted legislation introduced by Rep. Larry Buschon of Indiana, which passed the House in early-March, aimed at stopping fraud by requiring providers to enroll with states and report any terminated providers to the Centers for Medicare and Medicaid and require the states to pay back federal funds used toward improper payments.
Pennsylvania Rep. Joe Pitts also introduced legislation that would allow U.S. territories to exceed the cap placed on federal Medicaid funds when investing in Medicaid Fraud Control Units.
“Given that the Medicaid program consistently has the 2nd highest amount of waste, fraud, and abuse, more can and should be done to combat the occurrence of improper payments within the program,” AAF wrote. “While eliminating such payments will not solve the program’s long-term budgetary problems alone, the problem is large enough that successfully addressing it would generate substantial savings.”
Follow Juliegrace Brufke on Twitter
All content created by the Daily Caller News Foundation, an independent and nonpartisan newswire service, is available without charge to any legitimate news publisher that can provide a large audience. All republished articles must include our logo, our reporter’s byline and their DCNF affiliation. For any questions about our guidelines or partnering with us, please contact licensing@dailycallernewsfoundation.org.


